GOSH Charity-funded team engineers first lab-grown oesophagus in breakthrough for children’s surgery
20 Mar 2026, 11:31 a.m.
Groundbreaking research supported by Great Ormond Street Hospital Charity (GOSH Charity) has made huge strides towards personalised regenerative treatments for children born with life-threatening oesophageal conditions.
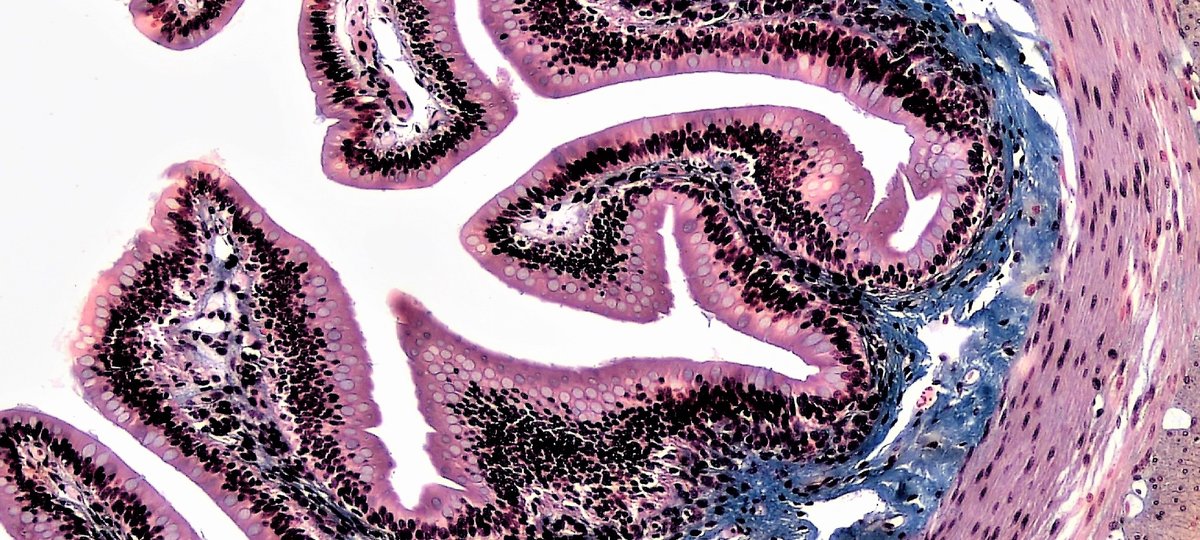
Scientists from Great Ormond Street Hospital (GOSH) and University College London (UCL) have created the first lab-grown oesophagus – the pipe that moves food from the throat to the stomach – and successfully transplanted it in a living animal model.
A new personalised treatment
Published today in Nature Biotechnology, the researchers showed, for the first time, that an oesophagus from a donor animal can be used as a base structure on which to grow a new section of an oesophagus using a recipient animal’s own cells – in a process called tissue engineering.
When implanted into a living animal model, the engineered oesophagus tissue was able to fully integrate into the digestive system, restoring function such as swallowing without the need to suppress their immune system. Immune suppressants are usually needed with donor tissue to prevent the recipient from rejecting the transplant.
The results could be transformational for children born with long-gap oesophageal atresia, a rare condition where the oesophagus doesn’t form properly and prevents food from passing to the stomach.
Children born with this condition will need to undergo surgery to repair the gap in the oesophagus. Surgical approaches currently include waiting for the oesophagus to grow more so the ends either side of the gap can be joined together, or using tissue from another organ such as the stomach or intestine to close the gap. This surgery is complex and can cause major breathing and gastrointestinal complications.
Tissue engineering would allow a replacement to be made without needing to use one of the patient’s existing organs, offering a less invasive option with a better chance at restoring long-term oesophageal function.
With further development, this work could result in an off-the-shelf structure that can be personalised for newborns or children with long-gap oesophageal atresia, restoring their ability to eat so they can continue to grow and live a healthy childhood.
Meet Casey

Casey on his toy car
When Casey was born, his parents, Sean and Silviya, were told he had a ‘gap’ in his oesophagus. He was immediately placed on a feeding tube and transferred to intensive care.
Over the next few months, Casey had several operations to try to close the gap and keep as much of his oesophagus tissue as possible. Unfortunately, these were unsuccessful.
Eventually, Casey was transferred to GOSH, where he underwent multiple operations – first to repair the gap, then, when the closure didn’t last, to have a tiny mesh tube, known as a stent, fitted. After a six-week stay in intensive care, he still couldn’t swallow on his own but was able to return home with a feeding tube.
Last year, Casey had his final surgery to repair the gap in his oesophagus. The recovery was easier this time, and he has since gone from strength to strength.
“He’s a champ,” Casey’s mum, Silviya says. “He’s in nursery now and, while he still has his feeding tube, he eats small meals and loves toast and berries, just like other toddlers he plays with.
“The surgery has left him with some damage to his vocal cords so he’s developing his speech and noise-making to catch up. Once he’s eating enough through his mouth, we’ll be able to take his tube out.”
Casey’s dad, Sean, says an operation that could transplant a working piece of oesophagus early in a child’s life would be “life changing”.
“We’ve had to learn things as new parents that we never considered would be part of our family life, from feeding him through a stomach tube to what to do if the hospital call with an urgent update in the middle of the night,” Sean says.
“He sleeps so well, which we think is likely because he spent his early months sleeping in a hospital cot, often with strangers. To look at him, he’s just amazing and we are very proud of him. What the team did for him was really a miracle.
Supporting future outstanding leaders in translational research

Dr Natalie Durkin
This research was supported by GOSH Charity through a Lewis Spitz Surgeon Scientist PhD studentship, granted to Dr Natalie Durkin, and a Translational Research Accelerator Grant, co-funded with LifeArc, awarded to Professor Paolo de Coppi.
"By funding my PhD Fellowship, GOSH Charity have been instrumental in advancing this work from a lab-based concept to a pre-clinical reality. I am enormously grateful for the opportunity to contribute to such groundbreaking research. The fellowship being named after Professor Lewis Spitz is particularly significant, as he dedicated so much of his work to improving care for children with oesophageal atresia."
About the Lewis Spitz Surgeon Scientist PhD Programme
The Lewis Spitz Surgeon Scientist PhD Programme aims to develop future surgeon scientist leaders with a demonstrable commitment to children’s surgery and excellence in translational research. The programme provides a full-time research opportunity for trainee surgeons to complete a PhD at UCL, receiving supervision from leading academics at the UCL Institute of Child Health and consultant surgeons at GOSH. The Lewis Spitz Surgeon Scientist PhD Programme is supported by GOSH Charity and the National Institute for Health and Care Research GOSH Biomedical Research Centre (NIHR GOSH BRC), although the NIHR did not directly fund the animal research mentioned in this article.