New understanding of childhood brain disorder
8 May 2024, 12:07 p.m.
A Cambridge based research team funded through GOSH Charity’s National Call has published findings which shed light on the cause behind Beta-propeller protein-associated neurodegeneration (BPAN), a rare brain disorder found in children.
This discovery could pave the way for new therapies for this untreatable, and often fatal, disease.
What is BPAN?
BPAN is a rare, life-limiting brain disorder which affects children, primarily girls.
The disease develops in two stages, beginning with seizures and developmental delays in infancy, followed by a decline in intellectual functioning and problems with movement. By early adulthood, people with BPAN develop dementia and Parkinson’s-like symptoms, such as slowed movements and difficulty walking.
There is currently no cure for BPAN; instead, treatments focus on managing the symptoms, however this does not stop the progression of the disease and sadly most people with BPAN do not live past middle age.
What causes BPAN?
BPAN is caused by a mutation to a gene called WDR45.
A gene is a segment of DNA which contains a set of instructions for making a specific protein. A gene mutation is like a typo in these instructions, which can cause the body to build the protein incorrectly or not at all. In BPAN, we know that the WDR45 gene mutation leads to the loss-of-function of the protein that it encodes, WIPI4.
The WIPI4 protein is involved in a process called autophagy, which controls how our cells remove waste. Previous work has therefore assumed that the loss of WIPI4 disrupts the autophagy process, leading to the development of BPAN. However, the exact mechanism behind BPAN is unconfirmed, which makes finding treatments for the condition challenging.
What did the team find?
Professor Rubinsztein and his team at the University of Cambridge used brain cells grown in the lab and zebrafish models to investigate what was happening at a cellular level in BPAN.
The team found that when they removed the WIPI4 protein from the brain cells, the brain cells died at a higher rate than normal. The team went on to investigate what was happening within the brain cells, and they found that the loss of the WIPI4 protein had a knock-on effect on a second protein which normally works with WIPI4 to maintain the health of the cell. Without the WIPI4 protein, this second protein changes its behaviour, and this triggers a process called ferroptosis. Ferroptosis is a type of programmed cell death, which can be very damaging to an organ like the brain.
Crucially, the team showed that ferroptosis was triggered without the involvement of the autophagy process, which was previously thought to be the main process involved in the disease. This is a new finding which opens the door for the discovery of treatments which can intervene in this ferroptosis pathway and prevent the development of the disease.

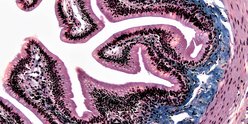
An image of the inside of a cell, highlighting the structures involved in BPAN (red = mitochondria, blue = endoplasmic reticulum, green = ATG2A). This image was taken using a technique called super resolution microscopy, which is a powerful way of viewing very small images in high resolution. More detail can be found in the research paper.
Making a difference through research
Prof Rubinsztein says:
“With diseases such as BPAN, because they are linked to a single gene mutation, you can really delve into the pathways that are affected and understand the biology. This gives us the opportunity to make a big difference to these diseases through research, however it also provides important insights into other diseases which share common pathways, in this instance other neurodegenerative diseases such as Alzheimer’s, Parkinson’s, Huntington’s and Motor Neurone Disease.”
Importance of funding
This study highlights the importance of funding research into paediatric rare diseases, which tend to be understudied.
GOSH Charity is committed to changing this through initiatives like our annual National Call, where researchers from across the UK are invited to apply for funding for paediatric research projects.
“I am very grateful to GOSH Charity for funding this work, it makes a big difference. The first funding we received for this project was from GOSH Charity, and that really catalysed what we have been doing.”
This study was funded in the 2021 round of the GOSH Charity National Call (formerly known as the GOSH Charity and Sparks National Call). The team also received support from UK Dementia Research Institute and the NIHR Biomedical research centre in Cambridge.